Eczema
Eczema (also known as dermatitis) is a dry skin condition. It is a highly individual condition which varies from person to person and comes in many different forms. It is not contagious so you cannot catch it from someone else.
In mild cases of eczema the skin is dry, scaly, red and itchy. In more severe cases there may be weeping, crusting and bleeding. Constant scratching causes the skin to split and bleed and also leaves it open to infection.
Eczema affects people of all ages but is primarily seen in children. Those who “grow out” of their eczema during early childhood may see it recur again in later life.
In the UK one in five children and one in twelve adults have eczema while eczema and contact dermatitis account for 84-90% of occupational skin disease.
Atopic eczema is a genetic condition based on the interaction between a number of genes and environmental factors. In most cases there will be a family history of either eczema or one of the other ‘atopic’ conditions ie asthma or hay fever.
Epidemiology and Classification
With a prevalence of 2-5% (in children and young adults approximately 10%), AEDS is one of the most commonly seen skin disorders. Atopy, the propensity of an individual to develop allergic reactions, is inherited, and atopy is a common finding in people with AEDS. The atopic (IgEmediated) diseases, AEDS, allergic asthma and allergic nasal and eye symptoms are genetically linked within families.
In some people with AEDS, true allergic reactions, those involving the IgE antibody, are clearly responsible for the development of the disease. There are however also many individuals in whom non-specific factors, such as skin irritants or psychological influences, appear to be important. AEDS consists of at least two different disorders. Patients belonging to the IgE-associated subgroup of AEDS will get worsening of their eczema upon contact with classical allergens, e.g., animal hairs. The other subgroups of AEDS are less well understood, but they are believed to result from internal mechanisms.
Symptoms and Signs, Differential Diagnosis
The symptoms of eczema vary depending on the type and severity. Symptoms of atopic eczema can include:
- Red, inflamed skin
- Dry, cracked skin
- itchy skin
- Small water blisters on the skin, particularly on the hands and feet - or the skin can become wet and weepy if it's infected
- Thickened areas of skin (lichenification) in places that are scratched frequently
Scratching the affected area damages the skin, causing it to bleed which can lead to infection.
Causes of eczema
You can't catch eczema. It doesn't spread from one person to another.
The exact cause of atopic eczema isn't fully understood at present. However, you can have a genetic, or inherited, tendency to develop the condition. Atopy means a family tendency to develop a variety of allergic conditions, including asthma, hay fever and eczema.
Sometimes, the symptoms 'flare up' for no obvious reason. But you may notice certain triggers that set off your, or your child's, eczema including:
- Chemicals, detergents, soap or shampoo
- Irritants such as pollen, house-dust mites, moulds or pet dander (tiny flakes of skin)
- Being "run down", for example if you're unwell
- Changes in hormone levels - the menstrual cycle and pregnancy can make eczema worse
- Stress
- High or low temperature or humidity - this leads to seasonal variation in eczema severity but sweating can also make eczema worse
- Rough or irritable fibres, such as wool
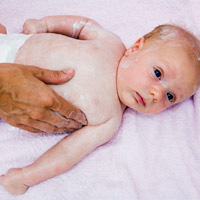
AEDS often begins with "cradle cap" in babies, after the first 3 months of life. As the baby becomes a toddler, the disease spreads to the face, outer elbows and knees, and the skin becomes oozing and crusting. Later on, eczema develops on the neck, hands, the inner elbows, and behind the knees. The skin becomes dry and scaly as a result of scratching and rubbing. In adults this may also result in weeping, itchy lumps and patches, the "prurigo form" of AEDS. New flare-ups of AEDS often start without obvious symptom, except for increased itching, which is followed by raised red lumps. These features can also occur in other skin disorders, and so to confirm a diagnosis the doctor will look for four of the following symptoms:
- Areas of skin showing the typical appearance of eczema;
- Early onset of symptoms of eczema;
- Typical location of the affected areas, bearing in mind the patient's age;
- Itching;
- Personal or family history of IgE-mediated allergic diseases - eczema, hay fever, asthma;
- Evidence of IgE-mediated reactions diagnosed by allergy skin prick tests or allergy blood tests.
Causes:
Abnormal immune and nervous system activity
Individuals with AEDS may have abnormal amounts of IgE antibody in their blood. This results from over-activity of some types of immune cells in the body, and under-activity of other cell types. Patients with AEDS are prone to develop a variety of infectious skin diseases caused by viruses, bacteria or fungal infections, and this has led to speculation that a defective immune system may be important in the development of AEDS. There may also be enhanced activity of the patient's nervous system, resulting in an increase in the chemicals that nerves release into the skin, causing the redness and itching.
Aeroallergens
Some patients with the IgE-associated variety of AEDS suffer from worsening of their skin symptoms after contact with certain airborne allergens, such as house dust mite, pollens, or animal hairs, and improve after appropriate allergen avoidance strategies are introduced.
Skin barrier and bacteria
Skin is a physical barrier that protects the internal structures and organs of the body, and it is thought that eczema may result from impairment of this barrier function. In AEDS, the skin loses its moisture content and becomes dry and scaly.
Compared to normal skin, there are several differences in the cells in the skin of atopic individuals, even when no eczema is present. A number of friendly bacteria live on human skin, but in individuals with AEDS, a harmful bacterium, Staphylococcus aureus, may grow, infecting the eczematous areas and causing further inflammation. This infection requires treatment with antibiotics. The skin may also be colonized by a yeast, Malassezia.
Eczema in practice
Eczema is a common condition. Atopic eczema affects about 10-20 per cent of schoolchildren and 3-5 per cent of adults in the UK, and it is getting more common.
An increase of between two- and five-fold has been seen over the past 30 years, for reasons that are far from clear.
It seems likely though that increasing exposure to allergens (protein substances to which people can become allergic) such as house dust mite and other environmental factors have been the main causes of this increase.
Although some older industrial practices have reduced the level of exposure of workers to irritant chemicals there are still plenty of examples of poor practice, or of inadequate care being taken at the individual level in handling materials known to potentially cause irritant contact eczema.
Even within the home environment ever more cleaning agents, solvents, detergents, oils and other materials potentially harmful to skin are easily available.
Eczema treatment is generally effective in most people but severe eczema can be difficult to clear. Good adherence to the basic elements of treatment will usually work well but only rarely can eczema be said to be curable.
It is unusual to be able to identify and eliminate a single agent causing the skin reaction and most of the time we have to settle for improving the condition rather than getting rid of it altogether.
REQUEST A FREE DEMONSTRATION IN YOUR HOME, NO OBLIGATION TO BUY